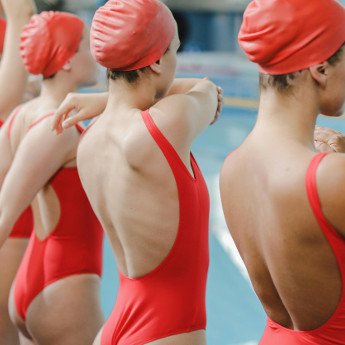By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Category : Stories
Charting a Different Course
Jeanne lost her mother when she was 25, and her aunt also had breast cancer. When Jeanne was diagnosed with triple-negative breast cancer (TNBC), her children were still very young. In her blog, www.triplenegatif.blogspot.com, Jeanne returns to the multiple aspects of the breast: that of the woman, the mother, the sick person, then the reconstructed breast. Heredity and lineage, but also faith, are questioned in a lyrical, almost poetic and soul-searching way.
From Diagnosis to “I Do”: Finding Life After Breast Cancer
I was just 27 years old, newly engaged and planning my wedding, when I was diagnosed with HER2+ Stage 2 breast cancer. Overnight, my world shifted from picking out flowers and venues to chemotherapy appointments, surgery dates, and a treatment plan that included chemo, surgery, and radiation.
The White T-shirt in My Drawer
I remember the day vividly: as a time of solidarity with a group of friends, colleagues and survivors. It was a great day, the streets filled with incredible energy and glorious pink accessories, sunglasses, feather boas and countless women, and a few brave men, all joined in a moment of support. I proudly wore that first T-shirt not knowing that 15 years later, I would be more than a supporter—I would also be a survivor of breast cancer.
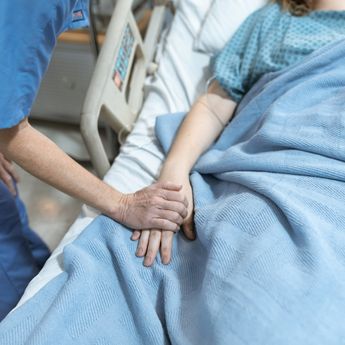
My Breast Cancer Surgery
When I was 15, I ended up in hospital with a ruptured, grapefruit-sized cyst on my left ovary. Two years later, another cyst required a second surgery. Years later, in my early 30s, a perforated appendix landed me back on the operating table. So, when I was diagnosed with breast cancer and surgery became part of my treatment plan, it felt old hat.
Still Burning: Cancer-free but the Heartburn Won’t Quit
Only after being diagnosed with breast cancer and undergoing surgery and treatment did the burning in my throat and chest—the uncomfortable, dry and always-on-fire feeling of heartburn—become a constant in my life. Single-digit years now, cancer-free, I'm still carting a container of Tums in my black Lululemon Everywhere Belt Bag.
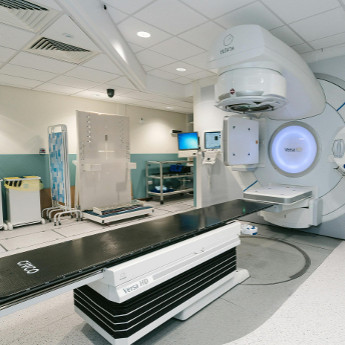
Radiation 411
Radiation therapy: two words that sounded surreal when I heard them attached to my cancer treatment plan. I knew what radiation was, technically, but I was clueless about what the actual experience would be like or how it would affect me. Mostly because my oncology team had described it and its potential side effects in vague terms. Apparently, this isn’t unusual for women like me who’ve been diagnosed with breast cancer.
Dancing Through Diagnosis, part 2
There was a total of three oncologists from different areas of care that I would meet along the way. Then there is my plastic surgeon! The beginnings of a joke. Three oncologists and a plastic surgeon go into a bar... If you have a good joke for this scenario, I would love to hear it. But this is the thought that keeps popping into my head every time I am told about my surgical team.
Dancing Through Diagnosis, part 1
As my towel brushed past the bottom of my right breast, I couldn’t help noticing that something didn’t feel right. Broken glass? It felt like broken glass. Is that possible? Could I have broken my boob? Can you break a boob? My mind began to swirl toward real questions then to ones that were clearly insane and made no sense... and yet, I asked them out loud... to myself... in the mirror.
How Surgery, Treatment & Tamoxifen Impact Your Sleep
I vividly remember the first night, after I found out I had breast cancer. I was lying in bed, wide awake with my eyes closed, listening to Trixie the cat purring beside me. My body was heavy, but my mind was wild, racing with thoughts of nothing and everything all mashed together. That was the beginning of a new kind of insomnia. Not the kind where you just can’t fall asleep, but the kind where sleep feels like something you used to do in a different lifetime but can’t access any more.
I Faced Cancer—Then I Faced Him. How One Man’s Bias Tried to Sink Me
Not long ago, I felt confident about my post-cancer status. Like I was finally rising above and beyond being just a breast cancer survivor. That I could actually do real-life things and shake off some of the lingering shadows. It felt good and empowering, and suddenly, I was ready to take on new challenges. So, I did, by swimming laps at the community centre pool. And boy, did I suck at it horribly.