By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Contributor : CBCN Team
Holiday Cheer?
Let me just start by saying, while writing, that I’m not a Grinch. I promise. That said, Christmas is not my favourite holiday. (Thanksgiving is, because it’s all about the gratitude, mashed potatoes and turkey.) Yet, after my breast cancer diagnosis, surgery and treatment, the only place I wanted to be for the holidays was with my family in Calgary. Being single and dealing with breast cancer’s day-to-day stressors alone, by myself with my cat, was overwhelming. So, my post-cancer-treatment Christmas was probably one of the most stress-free I’ve ever experienced. Maybe it’s because I didn’t have to make one decision for a solid week, that my family loved on me or because I didn’t cook a single meal, I don’t know. But it worked and when I returned to Toronto, despite the brain fog and Tamoxifen madness, I felt lighter.
Humour in Times of Crisis pt. 2 - Excerpts from Angel in the Marble
The minute you get a cancer diagnosis, you start looking for the magic cure. For me, this meant researching the hell out of the disease and revamping my lifestyle, exercise regime, spiritual practice, and diet. Within days, I knew the latest cancer breakthroughs and snake oil salesman’s remedy for the problem. And I took on the task of miraculous cure (and possible canonization) with a vengeance. Turmeric was the new gold standard. I popped four pills a day and drank Indian golden milk and turmeric lemon tea morning, noon, and night. My skin oozed Trumpian orange, my countertops glowed with permanent yellow stains, and man, did I feel good. I knocked back shots of apple cider vinegar chased by pomegranate juice. I downed hemp hearts, chia, flax, and bee pollen. My daughter Sonja arrived one day with the Holy Grail—a Vitamix— and it became my cauldron, a sacred vessel for preparing healing concoctions laced with kale, ginger, blueberries, and coconut water.
Fact: When I Look Good, I Do Feel Better
Growing up, every time I passed a mirror I would pause and stare at my reflection. I got busted for it too. A lot. My mom and aunties told me it wasn’t nice to look at myself, that it was vain or to cut it out—sometimes they said all three statements at the same time. To be clear, I wasn’t always admiring myself, I mean sometimes I was, but after I turned 12 and went to junior high school, my covert glances were more about me feeling insecure than anything else. I had to make sure I didn’t look weird, that my bobbed hair was tucked behind my left ear just so or that my highly Ten-O-Sixed skin wasn’t shining like a too-bright light. I was looking because I needed to reassure myself that I looked good. That I was good enough.
Giving Tuesday: The Impact of Your Donations
Tomorrow, November 29th is Giving Tuesday, the world’s largest generosity movement. Created in 2012, it was a simple idea: a day that encourages people to do good. Make someone smile, help a neighbour or a stranger, show up for an issue you care about, or give some of what you have to those in need. Giving Tuesday is a time when people come together to celebrate giving and participate in activities that support charities and non-profits; to thank, help, give, show kindness, and share with others. Donations made to CBCN help us fulfill these needs for people dealing with breast cancer, their loved ones, and caregivers.
Humour in Times of Crisis
The words “breast cancer” and “humour” are seldom in the same sentence. When it is revealed that someone has breast cancer, or any type of cancer, reactions are often in the form of sympathy, compassion, anger, denial, pity, or empathy; not jokes or laughter. While all emotions about being diagnosed or living with breast cancer are valid, having a sense of humour about it is often seen as being in bad taste or disrespectful. The role of humour in times of crisis generally gets a bad rap, whether it’s a natural disaster like Hurricane Katrina, or something personal, like a breast cancer diagnosis; however, it has been well documented that laughing about tragic or terrible things can make those things more easily borne, especially when that laughter is shared.
Why I Hate it When People Ask, “Are You Finished Treatment?”
I found a lump in April 2021 and a week later had a biopsy on my underarm and breast; on May 3, 2021, I was diagnosed with breast cancer. I was diagnosed Stage IV de novo by my oncologist after a single mastectomy on May 21, 2021. It was very difficult to hear the words “you have cancer”; it is a shock and something you never want to hear. I didn’t choose to have chemotherapy or radiation treatment; instead, I’m taking Ibrance and Letrozole.
Reason # 3 Why Cancer Still Sucks: It Makes You Feel So Sick
In this blog series, we present excerpts from Dr. David Stewart’s book A Short Primer on Why Cancer Still Sucks. In this post, Dr. Stewart breaks down and explains the most common symptoms of breast cancer.
FinNav Five: Experiences, Services, And Travel Assistance
Depending on your situation, your financial needs can come in different forms, from needing money to pay for rent, to needing help with paying for treatments, to requiring help with parking costs when you go for cancer treatments. To highlight the various types of programs listed in FinancialNavigator, we have put together this blogpost series.
Support Matters. How You Can Support Yourself & Other Breasties
During treatment, when I laid on the couch or in bed recuperating, I found support in a promise to seek and find more joy and purpose in my life once I resurfaced from feeling deep, deep under water. I kept it too, by returning to coaching competitive synchronized swimming athletes after a near 20-year hiatus from the sport. This has been incredibly rewarding. Along with the support of joy it continues to give me, coaching allows me to focus my energy and attention on others instead of on myself and to give back and support a community of young athletes I believe in very much.
We Are Not Counted
I am writing this from my hospital bed. One of many cancer-related hospital stays and visits. This hospital has become my second home. Fortunately, it’s a great hospital. That doesn’t mean I want to spend a lot of time here though. But that is inevitable when you have metastatic breast cancer, otherwise known as mBC. That is Stage IV cancer. Cancer that has travelled outside the breast and has metastasized into other areas of the body.
Breast Cancer at 36
I had a few benign tumors (Fibroadenomas) that I would check every six months via ultrasound, and I had one lump which was classified as benign and was told it was nothing to worry about. Three months after my last ultrasound, this lump grew very quickly and became painful. I went back for another ultrasound three months earlier than suggested, and it showed the lump was changing and growing extremely fast. I had a biopsy on June 8, 2022.
60 to 0 in Seconds - Being a Breast Cancer Patient
I am a woman. I am active. I am a mom. I am also living with metastatic breast cancer, and I am living well. I have been active all my life. I played a variety of sports ever since I was little, like competitive fastball and hockey. So, how could a super active, fit, and healthy individual, with no breast cancer or any other type of cancer in her family, all of a sudden be told she has stage IV breast cancer?
I Can Create My Reality
I read a lot. About everything, really, including Jackie Collins’ Hollywood Wives, which I’m about three decades late on, I know, but I just watched Lady Boss, The Jackie Collins Story on Netflix so here I am. The book is good too, in a dishy fantastical way, so naturally after 15 pages in I went back online and bought the sequel Hollywood Wives: The New Generation. But, that’s not the kind of reading I want to share. Books about the power of the mind, self-esteem, and mental health and how to create a positive reality are what I’m referring to. I like these types of books and have piles of them, because I honestly believe they work. I just wish I’d fallen back on them when I was initially diagnosed with breast cancer and going through surgery and treatment.
History of the BRCA 1 & 2 Genes
Before it was known that genes could be linked to various cancers, 1970s research focused largely on viruses and their role in the development of cancer. With the knowledge that family history had an impact on cancer risk, Mary-Claire King, an American geneticist, began to theorize possibilities beyond viruses and started her mission in identifying the cause of breast cancer running in families.
Breast Cancer Care for Lesbian and Bisexual Women
Who you are and where you live can greatly impact your access to care, and sexual orientation is no exception to this. Within the healthcare system, the LGBTQ+ community regularly experiences barriers when seeking adequate health services, and the effect of these barriers may result in poorer health outcomes. This leads to the question — does being a lesbian or bisexual woman affect your risk for breast cancer?
I Believe in Love For Endurance and Even, For Survival
I believe in love. Romantic love, yes. More importantly though, love of myself, love of my life and love of life. I’m writing this because love, my true and authentic belief in an all- encompassing love, is what gives me strength and get me through the day. I call it God’s love, but it can be called or seen as a higher power, the universe or whatever else works for you. It’s this that has helped me keep the faith that I would prevail over breast cancer.
Losses from mBC: Vision and Fertility
Five years ago, 2017, I had what I thought would be my last CT scan at the BC Cancer Agency. I was done. I busted out of there as if I was free, even though I had a mild concern about a weird, ongoing burp and GERD symptom. I was told this was anxiety and waited for the results thinking I would graduate from cancer world. This was the assumption from my medical team and something I thought could be true since it had been five and a half years since my early-stage diagnosis. Even though the fear of recurrence existed, I held strong like my oncologist did.
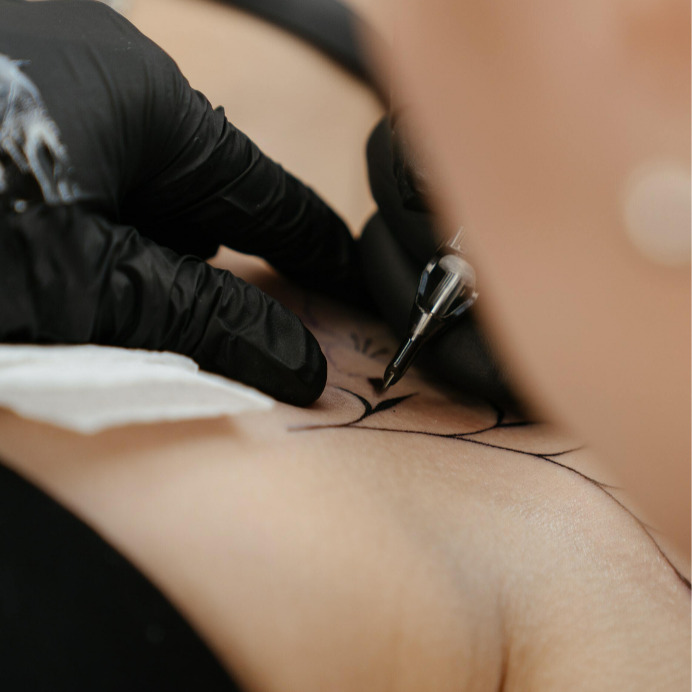
Considering a Mastectomy Tattoo? Here’s What You Need to Know
Following breast cancer surgery, there are a variety of options available to you. You may choose to live flat, have breast reconstruction, get implants, or use breast prostheses. Another option that you may have not considered or known about are mastectomy tattoos. Women who have gotten mastectomy tattoos following their breast cancer treatment have given a variety of reasons for getting them, including that they are a confidence boost following treatment, to cover scars, to create something beautiful, and to mark what they’ve been through.
To the Girl Standing in The Blue Hospital Gown, Part 2
I’m still scared and I’m still nervous, but I’m okay. I’m finding a sense of peace and calmness in all of this chaos. These past 42 days have been life changing. Being diagnosed and the end of a relationship has really tested my ability to find acceptance in everything. I continue to smile and laugh; life is truly incredible. The universe works in ways that I’ll never fully understand and in the darkest moments there is still light to be found.
Podcasts for Peace of Mind
I came to the Podcast game way late, like decades late. So when most people were tuning in on their morning commute to work, I was still listening to the mumbo jumbo in my head instead. Not that there’s anything wrong with this, I’ve always enjoyed my own company and I’m also a bit of a late bloomer which can translate into sometimes being a latecomer, so there’s that. But if I knew then how much I love a good podcast now, I’m fairly confident the time I spent waiting in Princess Margaret Hospital’s air-conditioned rooms would have passed by a lot quicker.